
Turning Hidden Inflammation into Something You Can Measure
Inflammation is a key driver in nearly every chronic disease – cardiovascular, metabolic, digestive, cognitive/neurological, auto-immune, arthritic, and more. Some forms progress silently for years, like endothelial inflammation that gradually scars arteries on the path to heart attack or stroke. Others, such as gastrointestinal (GI) disorders, are highly symptomatic, unpredictable, and difficult to trace to specific triggers.
While inflammation can come from many sources, diet is one of the most powerful and controllable. The problem is that broad rules about “anti-inflammatory eating” only go so far. People respond very differently to foods, stress, sleep, and environmental factors. That variability is why so many people spend years – and a lot of money – trying to figure out what’s actually driving their symptoms.
Nowhere is this frustration more obvious than in GI care. In a 2025 Quellios survey of 164 US adults managing chronic GI conditions, over half said they would “prefer virtually any new method” over what they’re doing today. That unmet need – and the clear desire for something simpler and more personalized – is what pushed us to build a better way: a method to detect food-triggered inflammation using only a smartphone.
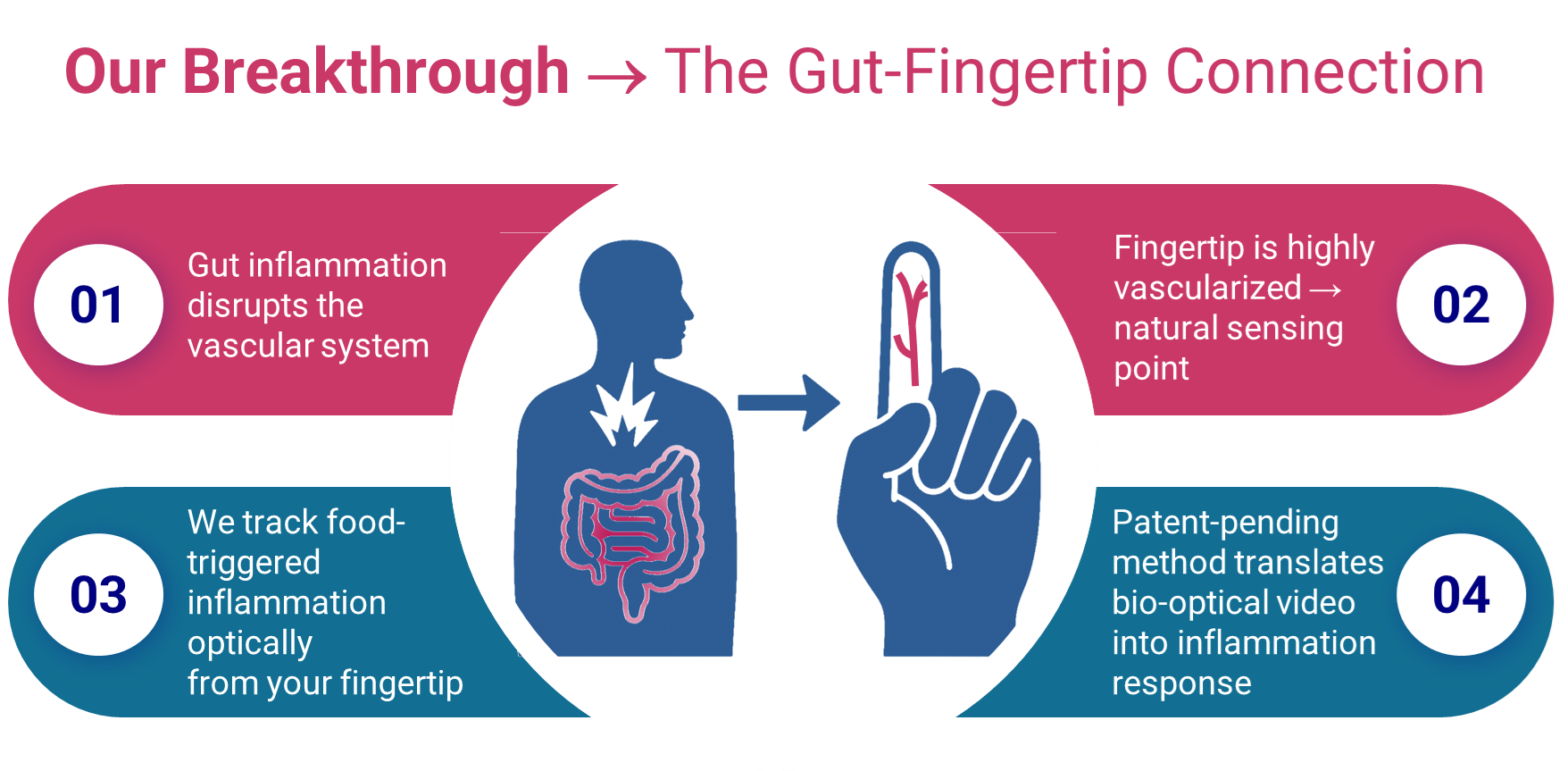
Inflammatory foods can irritate the gut locally and can also trigger a systemic, whole-body response that reaches the inner lining of the blood vessels – the endothelium. From a measurement standpoint, that’s useful. Unlike the gut, the endothelium can be assessed non-invasively and optically.
Because endothelial function is tightly tied to inflammation, rising inflammation reduces the vessels’ ability to dilate. Put simply: what you eat changes how your blood vessels behave, and those changes can be detected from a fingertip using light.
That’s the foundation of Quellios.

Snap → Sense → Connect the Dots
After you Snap a photo of your meal, the Quellios™ app breaks-down the food into macro- and micro-nutrients and scores the meal’s inflammation potential. From there, we estimate digestion timing and prompt you at the precise moment when a post-meal inflammatory response is most detectable. That’s when you take a Sense reading – a short fingertip video captured across multiple wavelengths of light. Because inflammation stiffens blood vessels and reduces their elasticity, those optical features shift in predictable ways.

Solving the Hard Problem: Confounders
Blood vessel behavior reflects many forces, not just inflammation. Physical activity, stress, sleep quality, air quality, hydration, illness, and overall inflammatory load can all influence the optical signal.
Heart rate variability (HRV), for example, correlates with inflammation and has been shown to predict flares in irritable bowel syndrome (IBS) – but HRV is also influenced by fitness, anxiety, sleep, and more. It’s too non-specific to isolate food-related inflammation on its own.
This is where the combination of Snap and Sense™ matters. Knowing what you ate and when you ate it makes the signals interpretable. On top of that, our physiological model is designed specifically to detect short-term inflammatory spikes and tease them apart from the noise of everyday life.
What We’ve Shown So Far
In our 20-person field study, Quellios has demonstrated the ability to:
- Detect food-triggered responses optically – via an iPhone camera
- Create personalized food-response profiles
- Identify signals correlated with personalized digestion timing and how specific nutrients affect it
- Identify body signals that precede self-reported food-related effects, sometimes by multiple days
- Correlate Sense measurements with known inflammatory food scores, such as the Dietary Inflammatory Index (DII) and glycemic load
- Identify personalized meal pairings that improve body responses shown, in scientific research, to be related to inflammation
This points toward a future where diet becomes a precision tool – not guesswork – and where people can actively improve digestive wellness with a piece of hardware they already own – their smartphone.
Why It Matters
Detecting bio-optical inflammation signals with a smartphone may feel like a leap, but the underlying biology is solid. When inflammation rises, the endothelium changes — and those changes appear in the optical signals we capture from the fingertip. The biggest challenge has always been filtering out everything else happening in the body. Our early data shows we’ve done exactly that.
By closing this loop with a patent-pending, data-driven method, we’re opening the door to something new: a truly personalized, day-to-day way to improve healthspan through food-as-medicine — and to prevent food-triggered symptoms before they start. Snap and Sense is coming in 2026, and if you’d like to experience it ahead of launch, we welcome you to join our Alpha waitlist.

References
- Vogel RA, Corretti MC, Plotnick GD. Effect of a single high-fat meal on endothelial function in healthy subjects. Am J Cardiol. 1997;79(3):350-354.
- Esposito K, Marfella R, Ciotola M, et al. Effect of a Mediterranean-style diet on endothelial dysfunction and markers of vascular inflammation in the metabolic syndrome: a randomized trial. JAMA. 2004;292(12):1440-1446.
- Anderson JW, Konz EC, Frederich RC, Wood CL. Long-term weight-loss maintenance: a meta-analysis of US studies. Am J Clin Nutr. 2001;74(5):579-584.
- Shivappa N, Steck SE, Hurley TG, Hussey JR, Hébert JR. Designing and developing a literature-derived, population-based dietary inflammatory index. Public Health Nutr. 2014;17(8):1689-1696.
- Brand-Miller J, Hayne S, Petocz P, Colagiuri S. Low-glycemic index diets in the management of diabetes: a meta-analysis of randomized controlled trials. Diabetes Care. 2003;26(8):2261-2267.
- Millasseau SC, Kelly RP, Ritter JM, Chowienczyk PJ. Determination of age-related increases in large artery stiffness by digital pulse contour analysis. Clin Sci. 2002;103(4):371-377.
- Elgendi M. On the analysis of fingertip photoplethysmogram signals. Curr Cardiol Rev. 2012;8(1):14-25.
- Takazawa K, Tanaka N, Fujita M, et al. Assessment of vasoactive agents and vascular aging by the second derivative of photoplethysmogram waveform. Hypertension. 1998;32(2):365-370.
- Tracey KJ. The inflammatory reflex. Nature. 2002;420(6917):853-859.
- Fung TT, McCullough ML, Newby PK, et al. Diet-quality scores and plasma concentrations of markers of inflammation and endothelial dysfunction. Am J Clin Nutr. 2005;82(1):163-173.
- Fewkes JJ, Kellow NJ, Cowan SF, Williamson G, Dordevic AL. A single, high-fat meal adversely affects postprandial endothelial function: a systematic review and meta-analysis. Am J Clin Nutr. 2022;116(3):699-729.
- McEniery CM, Wallace S, Mackenzie IS, et al. Endothelial function is associated with pulse pressure, pulse wave velocity, and augmentation index in healthy humans. Hypertension. 2006;48(4):602-608.
- Cooper TM, McKinley PS, Seeman TE, Choo TH, Lee S, Sloan RP. Heart rate variability predicts levels of inflammatory markers: evidence for the vagal anti-inflammatory pathway. Brain Behav Immun. 2015;49:94-100.
- Hirten R, Danieletto M, Landell K, et al. Physiological metrics collected from wearable devices identify inflammatory and clinical inflammatory bowel disease flares. Inflamm Bowel Dis. 2023;29(Suppl 1):S21-S22.
Leave a Reply